دانلود مقاله نابرابری های اجتماعی-اقتصادی در تاثیر سیاست های عمومی و پاندمی کووید 19 روی تغذیه انحصاری با شیر مادر
چکیده
هدف: در راستای ارزیابی تأثیر اضافه کردن 12 هفته مرخصی زایمان (ML) (2011)، استراتژی ارتقای پرداخت مبتنی بر عملکرد (P4P) تغذیه ی انحصاری با شیر مادر (2015)، و پاندمی کووید 19 در نابرابری های EBF در شیلی.
طراحی مطالعه: تجزیه و تحلیل های سری های زمانی منقطع و مختل شده (ITSAs).
روش ها: داده های گرد آوری شده ی EBF ملی از طریق شهرداری و براساس ماه از سال 2009 تا 2020 جمع آوری شدند. ما تأثیر سه رویداد در نابرابری های EBF را با استفاده از دو روش ارزیابی می کنیم: 1) ITSA طبقه بندی شده از طریق پنجک های SES شهری (Q1-Q5)؛ 2) محاسبه ی شاخص شیب نابرابری (SII) مربوط به EBF.
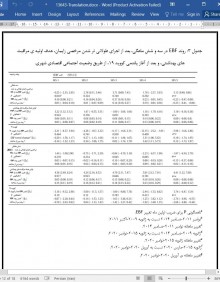
نتایج: رواج EBF در حوزه های شهری با SES پایین تر قبل و بعد از سه رویداد زمانی بالاتر بود. هیچ تأثیری در نابرابری های EBF بعد از طولانی کردن مرخصی زایمان (ML) مشاهده نشد. استراتژی P4P باعث افزایش EBF در شش ماهگی در تمامی پنجک های SES شد (اندازه اثر بین 4% و 5%)، اما در شهرهایی فقیرنشین تردر سطح بالاتری بود (SII: -0.36%, -1.05%). در طول پاندمی کووید 19، حوزه های شهری ثروتمندتر EBF نسبتا بالاتری را در شش ماه رواج آن نشان دادند (SII: 1.44%).
نتیجه گیری: تأثیر صفر افزایش مدت مرخصی زایمان در نابرابری های EBF را می توان با پایین بودن میزان مرخصی زایمان در میان اعضای وابسته به سیستم بهداشت عمومی توضیح داد (20%). استراتژی P4P مداخلات متعددی را دربر می گیرد که به نظر می رسید در افزایش EBF در میان پنجک های SES مؤثر باشد، اما بیشتر در پنجک های پایین تر. محدودیت های موجود در دسترسی به مراقبت های بهداشتی و خدمات درمانی در شهرهای فقیرنشین تر می توانند نابرابری های EBF در طول پاندمی کووید 19 را توضیح دهند.
مقدمه
مزایای متعدد تغذیه ی انحصاری با شیر مادر (EBF)، برای کودکان و مادران آن ها کاملا ثابت شده هستند.
کاواچی نابرابری های سلامت (HI) را به صورت توزیع نابرابر قابل برآورد، یا تفاوت های موجود در پیامد سلامت و بهداشت میان افراد یا گروه های تعریف شده شرح می دهد.
نابرابری های سلامت و بهداشت (HI) را می توان به عواملی نظیر عوامل فرهنگی، قومی و نژادی، تاریخی، اجتماعی-اقتصادی، منطقه ای، جغرافیایی، و تحصیلی ربط داد. این نابرابری ها در رواج EBF بین کشورها و درون آن ها نیز مشاهده شده اند.
کشورهای متعددی به معرفی سیاست های موفق در راستای افزایش رواج EBF پرداخته اند، مثل طرح بیمارستان دوستدار کودک؛ آموزش تخصصی برای متخصصان حوزه ی سلامت و بهداشت؛ مشاوره برای مادران و خانواده ی آن ها؛ مقررات مربوط به فروش و بازاریابی شیر بچه؛ و مرخصی زایمان با حقوق (ML). با این حال، تنها تعداد معدودی از این مداخلات کاهش نابرابری های EBF را نشان داده اند. بعضی از مطالعات نشان داده اند که ML می تواند در بالا بردن سطح EBF موفق عمل کند؛ هرچند، این سیاست ممکن است مطابق با وضعیت اجتماعی-اقتصادی (SES) نابرابری هایی داشته باشد.
در دهه ی گذشته، کشور شیلی دو سیاست را اعمال کرد که به صورت مستقیم و غیرمستقیم باعث ترویج EBF شدند (جدول تکمیلی 1 را مطالعه کنید): اضافه کردن 12 هفته به مرخصی زایمان در اکتبر 2011، که در مجموع این مرخصی به 24 هفته می رسد (پنج ماه و نیم) و استراتژی پرداخت مبتنی بر عملکرد (P4P) (که معمولا به صورت پاداش یا کمک هزینه ی مالی برای ایجاد انگیزه برای کادر مراقبت های بهداشتی و خدمات درمانی تعریف شده)، در ژانویه ی 2015. استراتژی P4P به منظور بهبود تحقق اهداف مراقبت های بهداشتی و خدمات درمانی در مراکز بهداشت و درمان (PHCC) طراحی شد. همچنین، پاندمی کووید 19 نابرابری های عمیق در دسترسی به خدمات بهداشت و درمان، افزایش وظایف روزمره ی مربوط به خانه میان زنان و افزایش بیکاری زنان را نشان داد. تمامی این عوامل می توانسته اند شیوه های EBF را تحت تأثیر گذاشته باشند.
نتیجه گیری
یافته های مشخص می کنند که هیچ نابرابری EBF بعد از اجرای طولانی تر شدن مرخصی زایمان شناسایی نشد، که می توان آن را با دسترسی پایین به ML در سیستم مراقبت های بهداشتی عمومی-وابسته و طول مدت ناکافی مرخصی زایمان (ML) توضیح داد. نتایج ما نیز نشان می دهند که استراتژی P4P در بالا بردن EBF در میان تمامی پنجک های اجتماعی-اقتصادی موفق عمل می کند، اما در سطح بالاتری در حوزه های شهری با SES پایین تر. پاندمی کووید 19 EBF در شش ماهگی را در حوزه های شهری ثروتمندتر افزایش داد، که برای شروع EBF کمتری داشت.
مطالعه ی ما نشان داد که تقویت پشتیبانی EBF در میان SES ضروری می باشد. افزایش طول مدت فعلی مرخصی زایمان، ارائه ی دسترسی منعطف تر به مرخصی زایمان و تقویت سیاست های ارتقای EBF به احتمال خیلی زیاد در رواج بالاتر EBF میان SES رشد کرده و شکوفا می شوند. مطالعات پیگیری روند EBF در طول پاندمی کووید 19 ضروری می باشند.
Abstract
Objective To assess the impact of the addition of 12 maternity leave (ML) weeks (2011), a pay for performance (P4P) exclusive breastfeeding (EBF) promotion strategy (2015), and the COVID-19 pandemic in EBF inequalities in Chile. Study design Interrupted time-series analyses (ITSAs).
Methods Aggregated national EBF data by municipality and month were collected from 2009 to 2020. We assess the impact of the three events in EBF inequalities using two procedures: 1. ITSA stratified by municipal SES quintiles (Q1-Q5); 2. Calculating the EBF slope index of inequality (SII).
Results The EBF prevalence was higher in lower SES municipalities before and after the three time-events. No impact in EBF inequalities was observed after the extended ML. The P4P strategy increased EBF at six months in all SES quintiles (effect size between 4% and 5%), but in a higher level in poorer municipalities (SII: −0.36% and −1.05%). During COVID-19, wealthier municipalities showed a slightly higher EBF at six months prevalence (SII: 1.44%).
Conclusion The null impact of the extended ML in EBF inequalities could be explained by a low access to ML among affiliated to the public health system (20%). The P4P strategy includes multiple interventions that seemed effective in increasing EBF across all SES quintiles, but further in lower quintiles. The restrictions in healthcare access in poorer municipalities could explain EBF inequalities during COVID-19.
Introduction
The multiple benefits of exclusive breastfeeding (EBF), for children and their mothers, are well established.1e4
Kawachi describes health inequalities (HI) as ‘measurable unequal distribution, or differences, on a health outcome across individuals or defined population groups’. 5
HI could be linked to cultural, ethnic, historical, socio-economic, regional, geographical, and educational factors, among others.6,7 These inequalities have also been observed in EBF prevalence, between and within countries.8,9
Several countries have introduced successful policies to increase EBF prevalence, such as the Baby-friendly Hospital Initiative; specialised training for health professionals; counselling for mothers and their families; regulation of formula milk sales and marketing; and paid maternity leave (ML).1,2,10 However, only a few of these interventions have documented a decrease in EBF inequalities.6,11,12 Some studies have reported that ML could be successful in increasing EBF; however, this policy might present inequalities according to socio-economic status (SES).13,14
In the past decade, Chile implemented two policies that directly and indirectly promoted EBF (see Supplemental Table 1): the addition of 12 weeks of ML in October 2011, bringing the total to 24 weeks (five and a half months) and a Pay for Performance (P4P) strategy (usually defined as financial incentives or rewards for healthcare workers), in January 2015.15,16 The P4P strategy was designed to improve healthcare goals accomplishment in public healthcare centres (PHCC).17,18 In addition, the COVID-19 pandemic revealed deep inequalities in access to healthcare services, increasing household duties in women's and a rise in female unemployment. All these factors could have affected EBF practices.19
Conclusion
Our findings highlight that no EBF inequalities were identified after the implementation of the extended ML, which could be explained by low ML access in public health system-affiliated and the insufficient duration of the ML. Our results also suggest that the P4P is successful in increasing EBF across all socio-economic quintiles, but in a higher level in lower SES municipalities. The COVID-19 pandemic increased EBF at six months in wealthier municipalities, which had lower EBF to begin with.
Our study showed that it is imperative to reinforce EBF support across SES. Increasing the ML current duration, providing more flexible ML access and enhance EBF promotion policies, are more likely to thrive in higher EBF prevalence across SES. Follow-up studies of the EBF trend during the COVID-19 period are required.
چکیده
مقدمه
روش ها
طراحی و تنظیم مطالعه
متغیرها و جمع آوری داده ها
نرخ تغذیه ی انحصاری با شیر مادر
وضعیت اجتماعی – اقتصادی (SES) شهری
متغیرهای کمکی
تغییرات و نوسانات فصلی
تعداد حوزه های شهری با داده های EBF
دسترس پذیری به مرخصی زایمان (ML)
تحلیل داده ها
استانداردهای اخلاقی
نتایج
بحث و گفتمان
نتیجه گیری
منابع
Abstract
Introduction
Methods
Study design and setting
Variables and data collection
Exclusive breastfeeding rates
Interventions (predictors)
Municipal SES
Covariables
Seasonality
Number of municipalities with EBF data
Accessibility to ML
Data analysis
Ethics
Results
Discussion
Conclusion
Author statements
Acknowledgements
Ethical approval
Financial support
Competing interests
Appendix A. Supplementary data
References
این محصول شامل پاورپوینت ترجمه نیز می باشد که پس از خرید قابل دانلود می باشد. پاورپوینت این مقاله حاوی 17 اسلاید و 5 فصل است. در صورت نیاز به ارائه مقاله در کنفرانس یا سمینار می توان از این فایل پاورپوینت استفاده کرد.
در این محصول، به همراه ترجمه کامل متن، یک فایل ورد ترجمه خلاصه نیز ارائه شده است. متن فارسی این مقاله در 6 صفحه (1700 کلمه) خلاصه شده و در داخل بسته قرار گرفته است.
علاوه بر ترجمه مقاله، یک فایل ورد نیز به این محصول اضافه شده است که در آن متن به صورت یک پاراگراف انگلیسی و یک پاراگراف فارسی درج شده است که باعث می شود به راحتی قادر به تشخیص ترجمه هر بخش از مقاله و مطالعه آن باشید. این فایل برای یادگیری و مطالعه همزمان متن انگلیسی و فارسی بسیار مفید می باشد.
بخش مهم دیگری از این محصول لغت نامه یا اصطلاحات تخصصی می باشد که در آن تعداد 40 عبارت و اصطلاح تخصصی استفاده شده در این مقاله در یک فایل اکسل جمع آوری شده است. در این فایل اصطلاحات انگلیسی (تک کلمه ای یا چند کلمه ای) در یک ستون و ترجمه آنها در ستون دیگر درج شده است که در صورت نیاز می توان به راحتی از این عبارات استفاده کرد.
- ترجمه فارسی مقاله با فرمت ورد (word) با قابلیت ویرایش و pdf بدون آرم سایت ای ترجمه
- پاورپوینت فارسی با فرمت pptx
- خلاصه فارسی با فرمت ورد (word)
- متن پاراگراف به پاراگراف انگلیسی و فارسی با فرمت ورد (word)
- اصطلاحات تخصصی با فرمت اکسل